
Extreme Weight Loss Devices: Safety and Effectiveness
 Elena MacLeod- Elena MacLeod is a fitness enthusiast who loves helping others achieve their health and wellness goals.
Elena MacLeod- Elena MacLeod is a fitness enthusiast who loves helping others achieve their health and wellness goals.In this detailed exploration, we delve into the safety profiles and effectiveness of a wide array of weight-loss techniques, spanning from unconventional injections like Botox and restrictive garments such as corsets to more invasive options including siphoning mechanisms and even parasitic infectio
In this detailed exploration, we delve into the safety profiles and effectiveness of a wide array of weight-loss techniques, spanning from unconventional injections like Botox and restrictive garments such as corsets to more invasive options including siphoning mechanisms and even parasitic infections.
Consider the scenario of an individual with moderate obesity engaging in moderate-intensity physical exercises, such as cycling or a brisk walk. Such activities typically result in the expenditure of around 350 calories within a single hour. However, many beverages, snack items, and various processed foods are ingested at a remarkably rapid pace, often delivering approximately 70 calories—or 293 kilojoules—every minute. This stark contrast means that just five minutes of consuming these items can completely negate the caloric burn achieved from an entire hour of dedicated exercise.
This is where innovative yet controversial devices like the AspireAssist siphon system come into play. Classified as a percutaneous gastrostomy apparatus, this device involves surgeons creating an incision directly into the stomach and establishing a fistula that extends through the abdominal wall to the exterior. Following each meal, users connect a specialized suction device to this external opening, allowing them to extract and expel the contents of their stomach, a process illustrated clearly in visual demonstrations available at the 0:47 mark in the associated video content on extreme weight-loss devices.
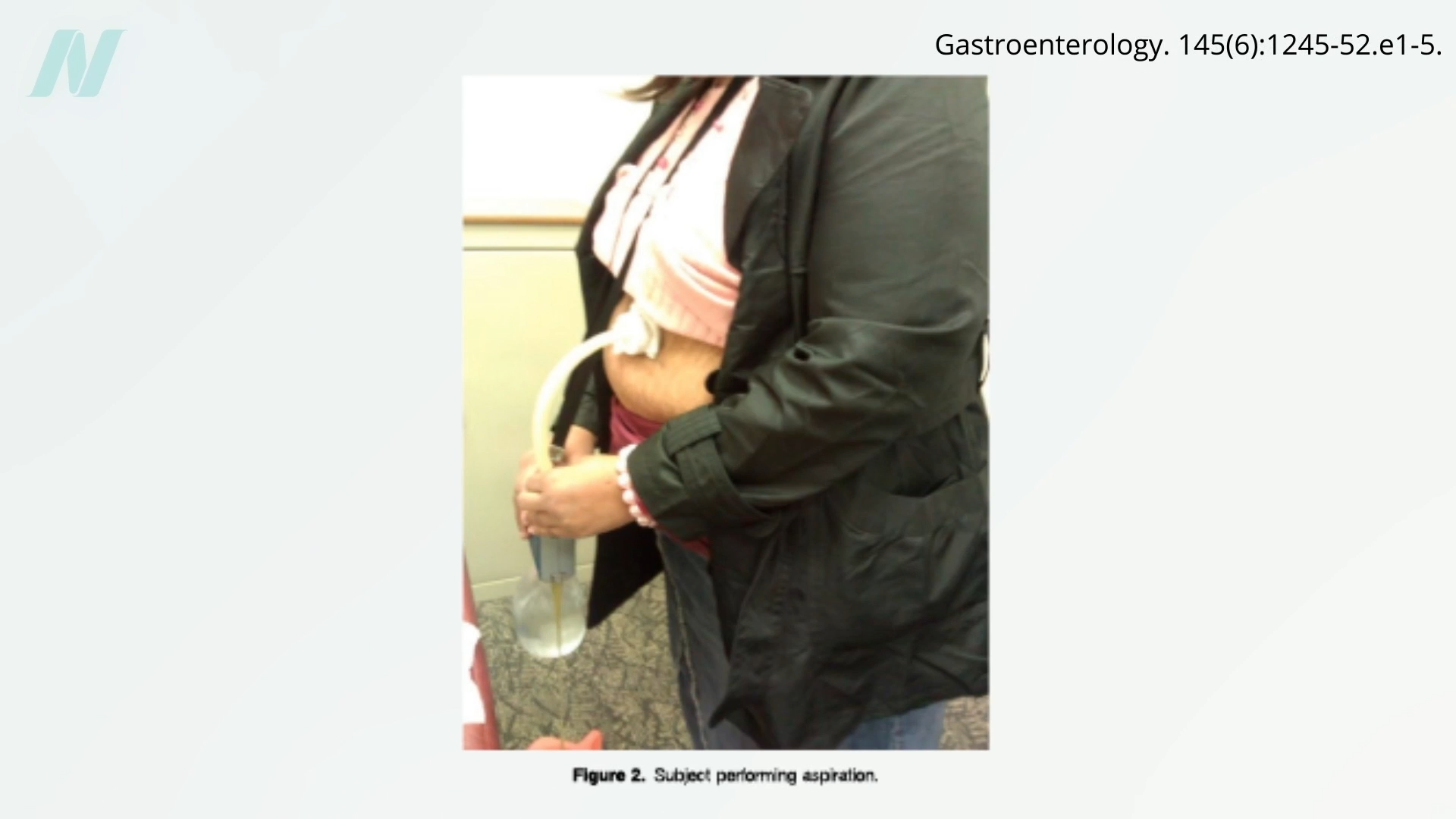
With this setup, individuals could theoretically indulge excessively in high-calorie treats like doughnuts, expel them via the stomach opening, and then proceed to consume additional servings without restraint. This allows for the paradoxical experience of having one's cake and devouring it multiple times over—once, twice, or even more.
The AspireAssist embodies a particularly bold approach to weight management, reminiscent of other quintessentially indulgent American culinary innovations, including gelatin-based salads, aerosol cheese products, and deep-fried candy bars. Clinical observations indicate that patients utilizing this device do achieve weight reduction, potentially due to the fistula disrupting the natural relaxation of the stomach muscles during eating. Furthermore, the procedure necessitates consuming substantial amounts of water and meticulously chewing food, practices that promote better hydration levels and decelerate the pace of ingestion, both of which contribute positively to weight control efforts. Participants in studies also reported shifting toward healthier food selections, motivated by the unappealing visual of aspirated gastric contents derived from unhealthy meals—especially since the extraction tubing is transparent, rendering greasy fried foods particularly repulsive when pumped out.
Every user of this system must supplement their intake of potassium, as the stomach fluids removed contain significant quantities of this essential mineral. Failure to do so could lead to potassium deficiency, a frequent issue observed in cases of bulimia nervosa. That said, the majority of side effects remain minor, primarily involving localized wound issues at the insertion site. More severe complications, such as abdominal abscess formations, occur infrequently. A primary advantage touted for the AspireAssist is its non-alteration of the gastrointestinal tract's inherent anatomy—a seemingly basic standard, yet one that holds relevance amid the unregulated landscape of contemporary weight-loss interventions. For contrast, examine the duodenal-jejunal bypass liner, another device in this category.
Traditional gastric bypass procedures function partly by excising segments of the small intestine, thereby bypassing them from the digestive pathway and reducing overall calorie absorption. As an alternative to extensive surgical resection, some approaches involve inserting a length of plastic tubing—roughly a couple of feet long—to coat the interior walls of the intestine. The EndoBarrier device, however, requires secure anchoring within the digestive system, achieved through the use of 10 barbed hooks that intentionally create lacerations. These hooks were responsible for the bulk of the 891 adverse events documented across 1,056 treated patients, affecting nearly 90 percent of participants. While grave injuries like esophageal perforations or liver abscesses are less common—occurring in approximately 1 out of every 27 cases—they underscore the inherent risks.
Critics have questioned the overall tolerability of the AspireAssist gastric pump, but during extensive research, an even more disconcerting endoscopic technique emerged: intestinal resurfacing. Rather than lining the intestinal interior with plastic to block nutrient uptake, why not thermally ablate the superficial layer of the duodenal mucosa? Essentially, this method entails burning away or resurfacing the intestinal lining through controlled heat application.
Medical professionals have experimented with injecting Botox directly into the stomach walls of obese patients, with the intention of inducing partial paralysis of the gastric musculature. The goal was to delay gastric emptying, prolong sensations of fullness, and facilitate sustained weight reduction. Unfortunately, these efforts proved unsuccessful in delivering the anticipated outcomes.
In a Swedish clinical trial, researchers randomized participants to wear corsets for 12 to 16 hours daily, every day of the week, over a nine-month period. This intervention failed to yield results, largely because subjects found the corsets excessively uncomfortable and discontinued their use—a predictable outcome given the restrictive nature of the garment.
Historical advertisements for sanitized tapeworms as a weight-loss solution date back to the early 1900s, promoted widely as an effortless method. Discoveries of live tapeworms in patients undergoing bariatric surgeries suggest that self-administering parasitic infections does not reliably lead to meaningful or sustained weight loss.
Turning to psychological tactics, consider leveraging disgust as a deterrent. A research study titled 'Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming' employed subliminal messaging to diminish appetite. Immediately prior to displaying images of nutritious foods, researchers flashed positive visuals—like a cluster of playful kittens—for a mere 20 milliseconds, too brief for conscious awareness but sufficient to subconsciously foster favorable associations. In contrast, before presenting high-calorie temptations such as ice cream, they exposed participants to repulsive imagery: a cockroach crawling on a pizza slice, vomit in a grimy restroom, or a severe burn injury. Remarkably, this approach succeeded; participants expressed diminished cravings for calorie-dense foods afterward, although direct behavioral testing was not conducted. The investigators posited that such subliminal aversion techniques could effectively counter the pervasive environmental cues encouraging overconsumption of unhealthy items.
Observers from other nations have viewed these American weight-loss experiments with a mix of amusement and concern, authoring commentaries such as 'Don't Let Them Eat Cake! A View from Across the Pond.' Publications in journals like Obesity Surgery have scrutinized U.S. innovations, including a piece questioning 'What Are the Yanks Doing?' in reference to implantable gastric stimulation. This involved surgically embedding electrodes into the stomach's muscular layer. When initial results disappointed, trials extended to colon electrical stimulation as another electrical intervention.
Even more alarming were investigations into repetitive electric brain stimulation for curbing food intake in humans. Although implanting deep-brain electrodes carries substantial procedural risks, researchers have long theorized about using targeted brain electrodes to suppress appetite. In one extreme study, surgeons drilled openings through the skulls of five obese subjects and inserted wires for exploratory electrostimulation. After identifying brain regions that triggered authentic hunger sensations upon probing, they applied sufficient electrical current to create electro-coagulatory lesions—essentially frying specific neural tissue. While preliminary animal studies with cats and monkeys showed promise, human trials revealed no significant weight loss from these invasive brain modifications. Fortunately, achieving healthy, enduring weight management does not necessitate such drastic neurological interventions, as sustainable strategies centered on evidence-based lifestyle adjustments offer superior paths forward.
Weekly Digest
Top articles delivered to your inbox every week.