
Milk Consumption and Parkinson's Risk Connection
 Elena MacLeod- Elena MacLeod is a fitness enthusiast who loves helping others achieve their health and wellness goals.
Elena MacLeod- Elena MacLeod is a fitness enthusiast who loves helping others achieve their health and wellness goals.Milk Consumption and Parkinson's Risk ConnectionParkinson’s disease represents a progressive neurodegenerative condition impacting the brain, affecting millions worldwide. Researchers have extensively examined the underlying causes, turning attention to various lifestyle elements. Among dietary choi
Milk Consumption and Parkinson's Risk Connection
Parkinson’s disease represents a progressive neurodegenerative condition impacting the brain, affecting millions worldwide. Researchers have extensively examined the underlying causes, turning attention to various lifestyle elements. Among dietary choices, consumption of dairy products emerges as the most robustly associated factor with elevated risk of developing this disorder. Notably, dairy stands alone as the sole food category repeatedly connected to heightened susceptibility to Parkinson’s across multiple investigations.
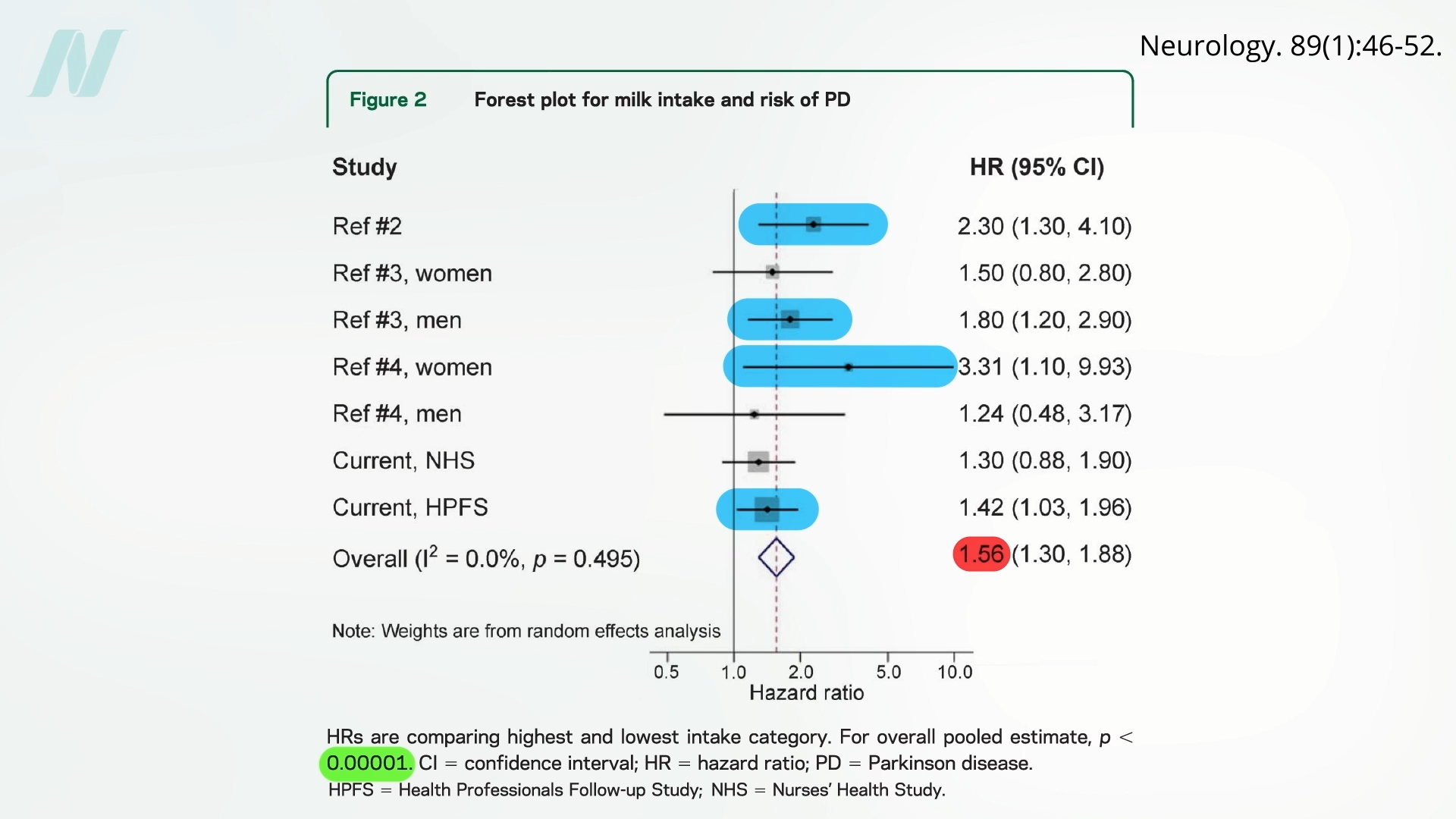
Extensive prospective studies, numbering five in total, have rigorously validated this association. These include prestigious cohorts such as the Nurses’ Health Study and the Health Professionals Follow-up Study from Harvard, which collectively tracked over 100,000 participants for several decades. Described as the most comprehensive analysis of dairy intake and Parkinson’s disease to date, this research scrutinized more than 1,000 fresh diagnoses. Every study identified a clear correlation between dairy consumption and Parkinson’s onset, with the majority demonstrating statistically significant results. Individuals consuming the highest quantities of milk exhibited approximately a 50 percent greater risk compared to those with minimal intake, backed by a p-value under 0.00001. This indicates an extraordinarily low probability—less than one in 100,000—of such findings occurring by chance alone.
While the connection between milk consumption and Parkinson’s incidence is firmly established, the precise mechanisms remain under scrutiny. One comprehensive review acknowledged the strong associations but noted a lack of definitive rationale at the time of its publication. However, subsequent research provided intriguing insights. A pivotal study explored midlife milk intake and its relation to neuron density in the substantia nigra upon death. This brain region is central to Parkinson’s pathology, where the primary culprit is the progressive degeneration and loss of specific dopamine-producing nerve cells. Symptoms typically manifest only after a substantial portion of these neurons have perished.
Investigators assessed milk consumption habits during participants’ middle years—specifically their 40s, 50s, and 60s—and later conducted detailed autopsies to quantify remaining neurons in the substantia nigra. Results revealed a striking pattern: neuron density peaked among those who abstained from milk entirely and reached its nadir in heavy consumers. This trend held across all examined quadrants of the brain region. Even excluding confirmed Parkinson’s cases, individuals averaging two cups—or about 473 milliliters—of milk daily displayed up to 40 percent fewer critical neurons in most areas of the substantia nigra.
What components in milk might contribute to such neuronal depletion? Analysis of heavy milk drinkers’ brains uncovered residues of heptachlor epoxide, a metabolite of the banned pesticide heptachlor, in nine out of ten samples. This pesticide, once used extensively in agriculture, contaminated dairy products through environmental persistence and bioaccumulation in cattle feed. The presence of these residues predominantly in the brains of high milk consumers offers a plausible causal pathway, suggesting that chronic exposure via dairy could drive the neuron loss central to Parkinson’s disease.
Beyond pesticides, alternative explanations merit consideration. For instance, certain animal products harbor alpha-synuclein, a protein implicated in Parkinson’s due to its propensity to misfold and aggregate, forming toxic clumps that damage neurons. Although evidence for significant alpha-synuclein in dairy remains tentative, trace quantities cannot be ruled out. Another compelling candidate is galactose, the simple sugar derived from lactose breakdown in the body. Galactose has been employed in laboratory settings to artificially accelerate brain aging, mimicking neurodegenerative changes.
Upon ingestion, galactose rapidly crosses into the brain within hours. At dosages exceeding 100 milligrams per kilogram of body weight, it triggers pathological changes in neural cells akin to those seen in Parkinson’s. Remarkably, this threshold is readily met or exceeded by routine consumption of two glasses of milk daily, positioning dairy as the predominant dietary source of galactose. Dopaminergic neurons, essential for averting Parkinson’s, appear particularly susceptible. These cells exhibit heightened vulnerability to oxidative stress, a key mechanism through which galactose inflicts damage.
This galactose hypothesis extends to broader health implications. Observational data link higher milk intake to increased overall mortality, independent of fat content. Even skim milk, devoid of saturated fats, retains full lactose levels, thus delivering equivalent galactose loads. Attempts to circumvent this via lactose-free options like Lactaid prove ineffective; the added lactase enzyme hydrolyzes lactose into glucose and galactose preemptively in the packaging, yielding the same galactose intake.
Cognitive ramifications further underscore potential risks. Midlife milk consumption correlates with accelerated cognitive decline in later years. Laboratory models routinely utilize D-galactose, a lactose metabolite, to replicate age-related cognitive impairment via oxidative stress pathways. Compared to rare milk drinkers, those averaging over one glass—or 237 milliliters—daily face elevated odds of global cognitive function deterioration.
Key Takeaways from Dairy and Parkinson’s Research
- Dairy products uniquely correlate with elevated Parkinson’s risk among food groups. Large-scale studies consistently show high milk consumers may incur roughly 50 percent greater risk versus low consumers.
- Autopsy findings indicate midlife two-cup daily milk drinkers retain up to 40 percent fewer substantia nigra neurons, the epicenter of Parkinson’s-related cell death.
- Heptachlor epoxide pesticide residues appeared in 90 percent of heavy milk drinkers’ brains, implicating contaminated dairy in neuron destruction.
- Galactose from milk accesses the brain swiftly, provoking oxidative damage at everyday doses from two glasses, fostering brain aging and cognitive deficits.
These findings collectively highlight dairy’s complex interplay with brain health. While pesticides like heptachlor epoxide represent historical contaminants—now largely phased out—endogenous milk components such as galactose persist as inherent concerns. Dopaminergic neurons’ oxidative sensitivity amplifies galactose’s threat, potentially eroding neural reserves over decades. Epidemiological patterns, from cohort tracking to postmortem analyses, converge on milk as a modifiable risk vector. Individuals seeking to mitigate Parkinson’s odds might weigh reducing dairy reliance, favoring plant-based alternatives that sidestep these pitfalls without sacrificing nutrition.
Further bolstering the galactose angle, experimental paradigms affirm its neurotoxic profile. Administered to rodents, D-galactose reliably precipitates cognitive deficits, neuronal apoptosis, and oxidative markers mirroring human neurodegeneration. Human equivalence calculations confirm dietary attainability: a 70-kilogram adult ingesting 473 milliliters of milk absorbs roughly 12 grams of galactose, surpassing the 7-gram threshold for brain effects. This metabolic burden accumulates, particularly in aging brains with waning antioxidant defenses.
Pesticide residues, though diminished post-ban, illustrate dairy’s vulnerability to toxins. Heptachlor’s lipophilic nature concentrates it in milk fat, with epoxide persisting in neural tissue. The 90 percent detection rate among high consumers underscores bioaccumulation risks from chronic exposure. Modern dairy, while safer, prompts vigilance against emerging contaminants like PFAS or antibiotics.
Alpha-synuclein’s tentative dairy link draws from meat parallels, where cooking liberates prion-like strains propagating pathology. Dairy’s lower protein content tempers this, but pasteurization or processing might exacerbate misfolding. Rigorous testing awaits, yet the convergence of multiple pathways—pesticides, galactose, proteins—renders dairy’s risk profile compelling.
Mortality data reinforce implications: high milk intake portends shorter lifespans across fat variants, implicating non-lipid factors like galactose-driven inflammation or glycation. Cognitive trajectories align, with milk-linked declines spanning memory, executive function, and processing speed. Public health strategies might prioritize awareness, empowering informed choices amid pervasive dairy promotion.
Weekly Digest
Top articles delivered to your inbox every week.